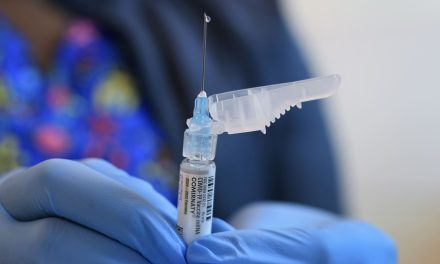
How AI is used to detect cancer that doctors miss

dr Éva Ambrózay, a radiologist with more than two decades of experience, peered at a computer monitor showing a patient’s mammogram in a darkened room at Bács-Kiskun County Hospital outside Budapest.
Two radiologists had previously said that the X-ray showed no evidence that the patient had breast cancer. But dr Ambrózay looked closely at several areas of the scan circled in red that the artificial intelligence software had flagged as potentially cancerous.
“That’s something,” she said. She soon ordered the woman called back for a biopsy, which will take place within the next week.
Advances in AI are beginning to deliver breakthroughs in breast cancer screening by detecting the signs doctors miss. So far, the technology is showing an impressive ability to detect cancer at least as well as human radiologists, so early results and radiologists are one of the most tangible signs yet of how AI can improve public health.
Hungary, which has a robust breast cancer screening program, is one of the largest testing areas for the technology on real patients. AI systems have been rolled out in five hospitals and clinics that perform more than 35,000 screenings a year from 2021 and are now helping to look for signs of cancer that a radiologist may have missed. Clinics and hospitals in the United States, Great Britain and the European Union are also beginning to test the systems or provide data to support the development of the systems.
AI use is increasing as the technology has become the center of a Silicon Valley boom, with the release of chatbots like ChatGPT showing how AI has a remarkable ability to communicate in human-like prose — sometimes with worrying results. Based on a similar shape used by chatbots, which is modeled after the human brain, breast cancer screening technology shows other ways AI is invading everyday life.
Widespread deployment of cancer detection technology still faces many hurdles, doctors and AI developers said. Further clinical trials are required before the systems can be more widely deployed as automated second or third readers for breast cancer screening, beyond the limited number of sites where the technology is currently being used. The tool must also demonstrate that it can provide accurate results for women of all ages, ethnicities, and body types. And the technology needs to prove it can detect more complex forms of breast cancer and reduce false positives that aren’t cancerous, radiologists said.
The AI tools have also sparked debate over whether they will replace human radiologists, with the makers of the technology facing regulatory scrutiny and opposition from some doctors and healthcare facilities. For now, those fears seem overblown, with many experts saying the technology is only effective and trusted by patients when used in conjunction with trained doctors.
And ultimately, AI could be life-saving, said Dr. László Tabár, a leading mammography educator in Europe, who said he was convinced by the technology after reviewing its performance in breast cancer screening from multiple providers.
“I dream of the day women will walk into a breast cancer center and be like, ‘Do you have AI or not?'” he said.
Hundreds of images per day
In 2016, Geoff Hinton, one of the world’s leading AI researchers, argued that the technology would eclipse a radiologist’s skills within five years.
“I think if you work as a radiologist, you’re like Wile E. Coyote in the cartoon,” he told The New Yorker in 2017. “You’re already over the edge of the cliff, but you haven’t checked down yet. There is no floor underneath.”
Mr. Hinton and two of his students at the University of Toronto built an image recognition system that could accurately identify common objects like flowers, dogs and cars. The technology at the heart of their system – a so-called neural network – is modeled on how the human brain processes information from different sources. It’s used to identify people and animals in images posted to apps like Google Photos, and allows Siri and Alexa to recognize the words being spoken. Neural networks also powered the new wave of chatbots like ChatGPT.
Many AI evangelists believed that such technology could be easily applied to detect diseases like breast cancer in a mammogram. In 2020, there were 2.3 million breast cancer diagnoses and 685,000 deaths from the disease, according to the World Health Organization.
But not everyone agreed that replacing radiologists would be as easy as Mr Hinton had predicted. Peter Kecskemethy, a computer scientist and co-founder of Kheiron Medical Technologies, a software company developing AI tools to help radiologists detect early signs of cancer, knew the reality would be more complicated.
Mr. Kecskemethy grew up in Hungary and spent some time in one of Budapest’s largest hospitals. His mother was a radiologist, which gave him first-hand insight into the difficulties of finding a small malignancy in an image. Radiologists often spend hours every day in a dark room looking at hundreds of images and making life-changing decisions for patients.
“It’s so easy to miss tiny lesions,” said Dr. Edith Karpati, the mother of Mr. Kecskemethy, who is now Director of Medical Products at Kheiron. “It’s not possible to stay focused.”
Mr. Kecskemethy, along with Kheiron’s co-founder Tobias Rijken, an expert in machine learning, said AI should help doctors. To train their AI systems, they collected more than five million historical mammograms from patients with known diagnoses, provided by clinics in Hungary and Argentina, as well as academic institutions such as Emory University. The London-based company also pays 12 radiologists to tag images with special software that teaches AI to recognize a cancerous growth based on its shape, density, location and other factors.
From the millions of cases fed into the system, the technology creates a mathematical representation of normal and cancerous mammograms. With the ability to look at each image in more detail than the human eye, it then compares this baseline to find abnormalities in each mammogram.
Last year, after testing more than 275,000 breast cancer cases, Kheiron reported that his AI software matched the performance of human radiologists when acting as a second reader of mammography scans. It also reduced the radiologists’ workload by at least 30 percent because it reduced the number of X-rays they needed to read. In other findings from a Hungarian clinic last year, the technology increased cancer detection rates by 13 percent as more malignancies were identified.
dr Tabár, whose techniques for reading a mammogram are commonly used by radiologists, tried the software in 2021 by tracking down several of the most difficult cases of his career where radiologists missed signs of developing cancer. In any case, the AI discovered it.
“I was shockingly surprised at how good it was,” said Dr. Tabar. He said that he had no financial ties to Kheiron when he first tested the technology and has since received a consulting fee for feedback to improve the systems. Systems he’s tested from other AI companies, including South Korea’s Lunit Insight and Germany’s Vara, have also yielded encouraging detection results, he said.
Proof in Hungary
Kheiron’s technology was first used on patients in 2021 at a small clinic in Budapest called MaMMa Klinika. After a mammogram is completed, two radiologists check it for signs of cancer. Then the AI either matches up with the doctors or marks areas to check again.
At five MaMMa Klinika sites in Hungary, 22 cases where the AI identified a cancer missed by radiologists have been documented since 2021, with around 40 others currently being reviewed.
“This is a major breakthrough,” said Dr. András Vadászy, Director of the MaMMa Klinika, who is represented by Dr. Karpati, the mother of Mr. Kecskemethy, was introduced to Kheiron. “If this process saves a life or two, it will be worth it.”
Kheiron said the technology works best alongside doctors, not in their place. The Scottish National Health Service will use it as a supplemental reader for mammography scans at six sites, and it will be present at around 30 English National Health Service breast cancer screening sites by the end of the year. Oulu University Hospital in Finland plans to use the technology as well, and a bus will be traveling through Oman this year to carry out breast cancer screenings using AI
“An AI-plus doctor should replace the doctor alone, but an AI should not replace the doctor,” said Mr. Kecskemethy.
The National Cancer Institute has estimated that about 20 percent of breast cancer cases are missed on screening mammograms.
Constance Lehman, a professor of radiology at Harvard Medical School and chief of breast imaging and radiology at Massachusetts General Hospital, urged doctors to keep an open mind.
“We’re not irrelevant,” she said, “but there are tasks that can be done better with computers.”
At Bács-Kiskun County Hospital outside of Budapest, Dr. Ambrózay, she was initially skeptical about the technology – but was quickly convinced. She pulled out the X-ray of a 58-year-old woman with a tiny tumor that was detected by the AI and that Dr. Ambrózay could hardly see.
The AI saw something, she said, “that seemed to appear out of nowhere.”