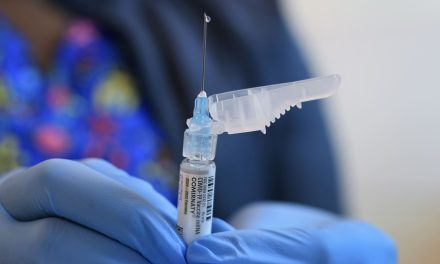
Excruciating leg pain hobbled her for weeks. What was wrong?

When her medical assistant questioned the patient, Kocharla carefully reviewed her notes and test results. This type of neuropathy was not uncommon in autoimmune diseases. Sjogren’s syndrome and lupus were probably the most common, but there were others. She had to keep an open mind and watch for other symptoms that might narrow the field. This kind of mysteries was one of the great joys of working in rheumatology. The PA summarized their findings and Kocharla entered the examination room and introduced herself to the middle-aged woman and her husband. She had heard about the aching legs, Kocharla began, but what else happened? So much! She was in pain all over and had lost more than 20 pounds in the last few months. Maybe the pain had robbed her of her appetite, but she hadn’t felt very well since she had asthma two years ago. This seemed to get the rheumatologist’s attention – which surprised the patient. She had told many doctors about her sudden asthma, but none seemed to care. Until now.
A new list of symptoms
“Wait a minute,” Kocharla said after hearing that part of the story. She turned to her laptop and typed something into it. Then she handed it to the patient. “Do any of these symptoms sound familiar?” she asked.
The patient looked through the list.
Fatigue: Sure, but who isn’t tired? Weight loss: check. Swollen lymph nodes: check. Muscle pain: check.
And she had the asthma and the numbness and weakness in her left foot and right big toe. “I think you have something called eosinophilic granulomatosis with polyangiitis,” Kocharla said. EGPA was formerly called Churg-Strauss syndrome after two doctors, Jacob Churg and Lotte Strauss, who first described the condition in 1951. The disease is linked to increased levels of white blood cells called eosinophils — the cells that respond to allergic reactions. Somehow, these cells become involved in the destruction of small blood vessels throughout the body. This causes numbness and loss of strength and reflexes. These cells can attack blood vessels anywhere in the body. It’s not clear what triggers this disorder, but it is a devastating, sometimes fatal, disease.
Kocharla checked the patient’s blood work. In fact, her eosinophil count was quite high – eight times the normal level. The rheumatologist had never seen this disease in a patient, but had certainly heard about it from her colleagues. A biopsy would be needed to confirm the diagnosis, but this could permanently damage the already injured nerve. This patient met almost all diagnostic criteria. She started the patient on a high dose of prednisone to blunt the attack caused by white blood cells. But because she had never seen a patient with EGPA, she wanted someone with more experience to confirm the diagnosis: She sent the patient to the Mayo Clinic in Rochester, Minnesota for a second opinion. Even before the patient visited the doctors in Mayo, she had no doubt that Kocharla was right. After just a week on steroids she felt great. The pain was gone. She could sit and stand. The level of eosinophils decreased to normal. She could go back to work. Mayo’s rheumatologist had seen many cases of EGPA and agreed with Kocharla’s diagnosis. They started on a second immunosuppressive drug.
Following her instinct as a reporter, the patient began researching the disease. One article suggested that walking can help control this and other autoimmune diseases, so the patient started taking walks. They average six to seven miles a day. It has allowed her doctors to lower her doses of medication, and she says that despite being ill – sicker than ever in a very real way – she has never felt healthier.
Lisa Sanders, MD, is a contributing writer for the magazine. Her latest book is Diagnosis: Solving the Most Baffling Medical Mysteries. If you have a solved case you want to share, write to her at Lisa.Sandersmdnyt@gmail.com.